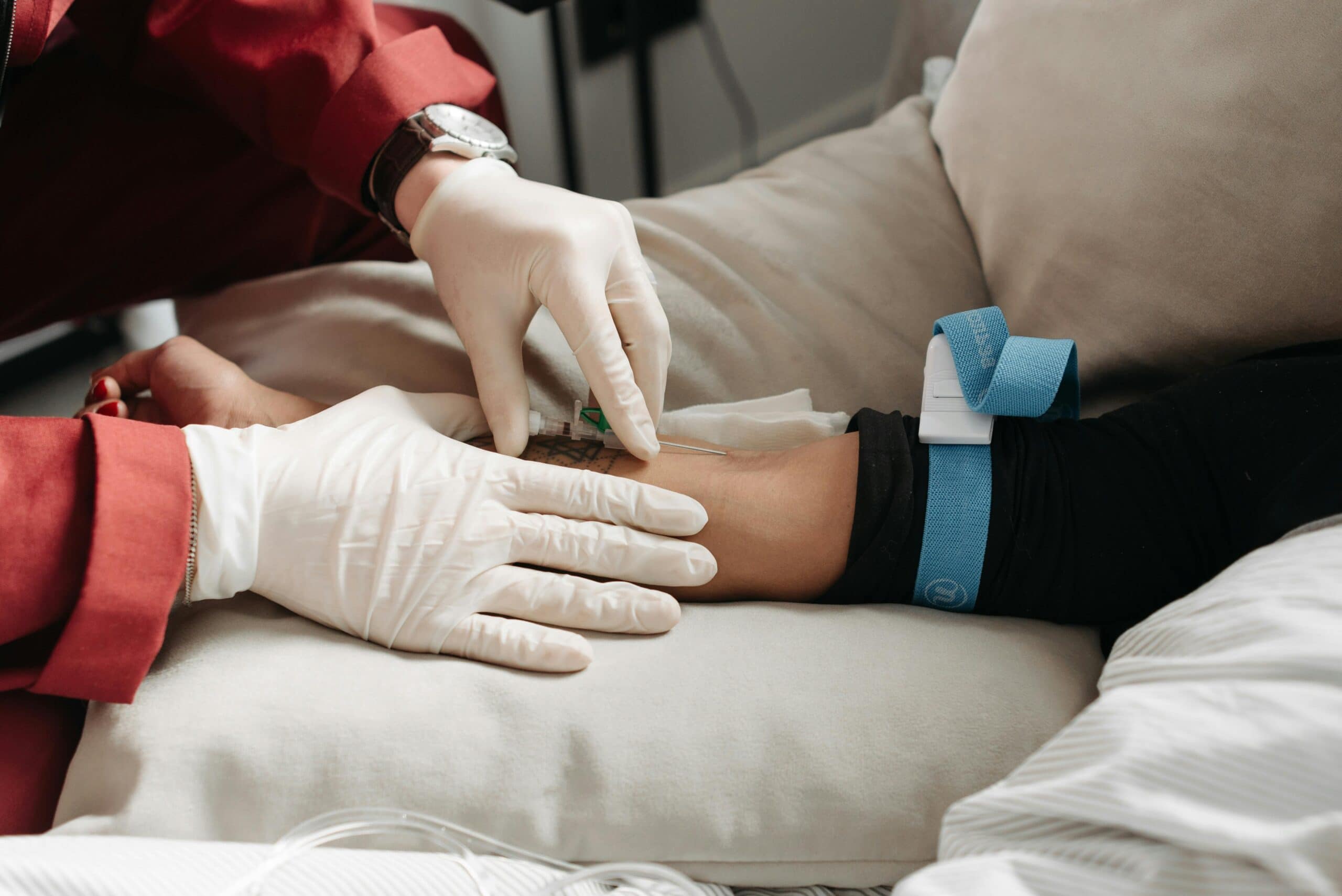
Not every medical bill can be avoided, but the choices you make before getting care can affect the final cost more than most people realize. The same minor illness or injury can end up costing completely different amounts depending on where you go and how the visit is handled. A quick decision in the moment can sometimes mean paying far more than necessary, even for routine care.
1. Skipping preventive visits that are covered at no cost

Many plans, including a lot of HDHPs, cover in-network preventive services—like annual checkups and certain screenings—without copays or deductibles.
If you avoid checkups “to save money,” small issues can turn into bigger, more expensive problems later. It’s worth checking your plan’s preventive list so you don’t leave fully covered care on the table.
2. Booking with out-of-network providers when an in-network option exists

Out-of-network care usually means higher deductibles, higher coinsurance, or no coverage at all. Even a simple office visit can double or triple in cost once it’s out of network.
Before you book, confirm the provider, the facility, and any associated labs or imaging sites are in-network. Don’t assume—network lists change.
3. Heading straight to the ER for things urgent care or telehealth can handle
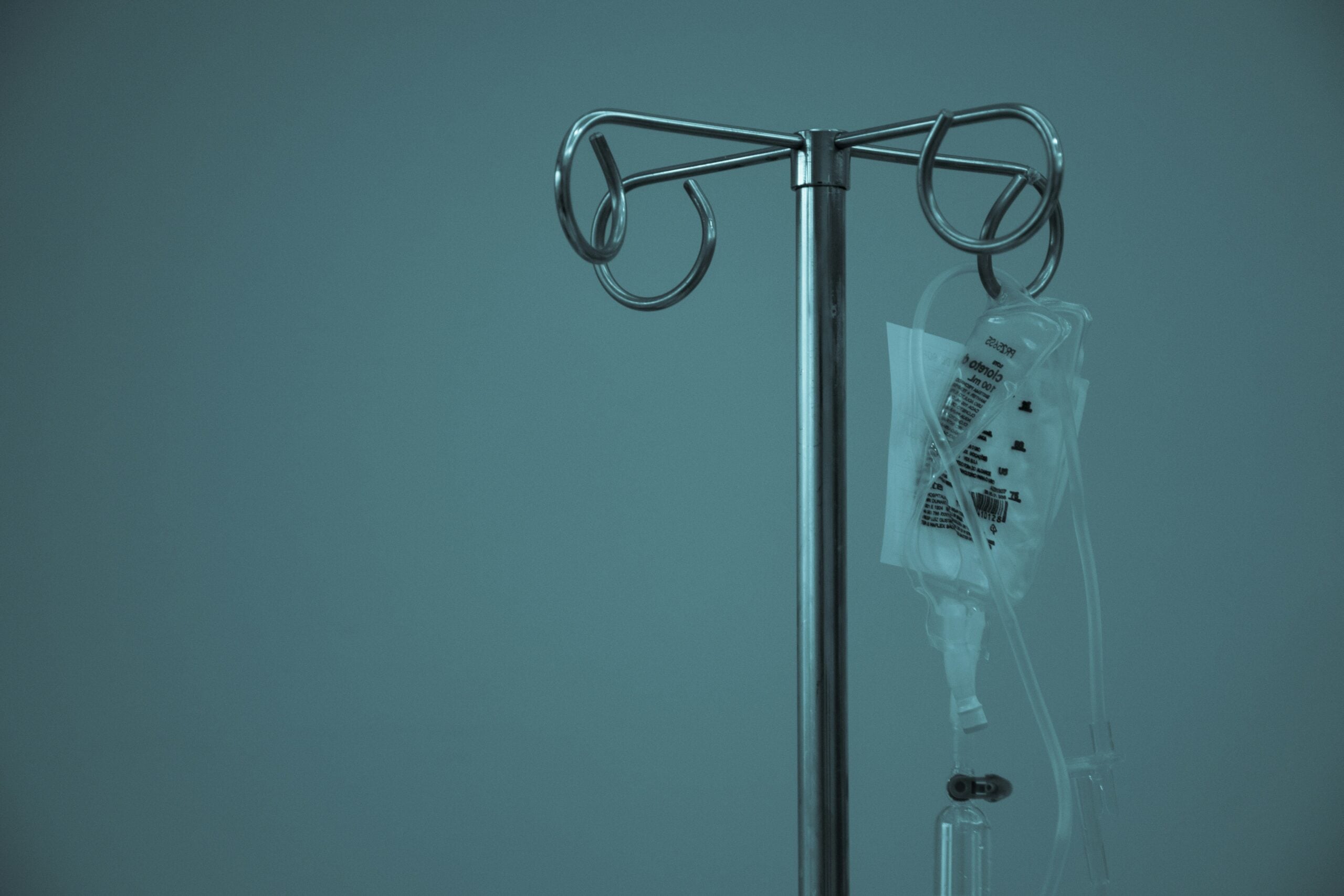
Emergency rooms are for true emergencies—and they’re priced that way. ER visits often run in the thousands of dollars, while urgent care is usually in the low hundreds and virtual visits can be even cheaper.
If it’s not life-threatening and you can safely choose, check your plan’s nurse line or care guide to see if urgent care or a virtual visit is appropriate.
4. Turning a simple issue into a long, multi-topic visit

Bringing a laundry list of unrelated issues to one appointment can sometimes bump the visit up to a higher billing level, which means a higher allowed charge and bigger share for you.
You don’t have to separate everything, but if you have one big concern and five small ones, it can be worth asking how the visit will be billed and whether a follow-up makes more sense.
5. Skipping referrals or seeing specialists without checking how your plan works
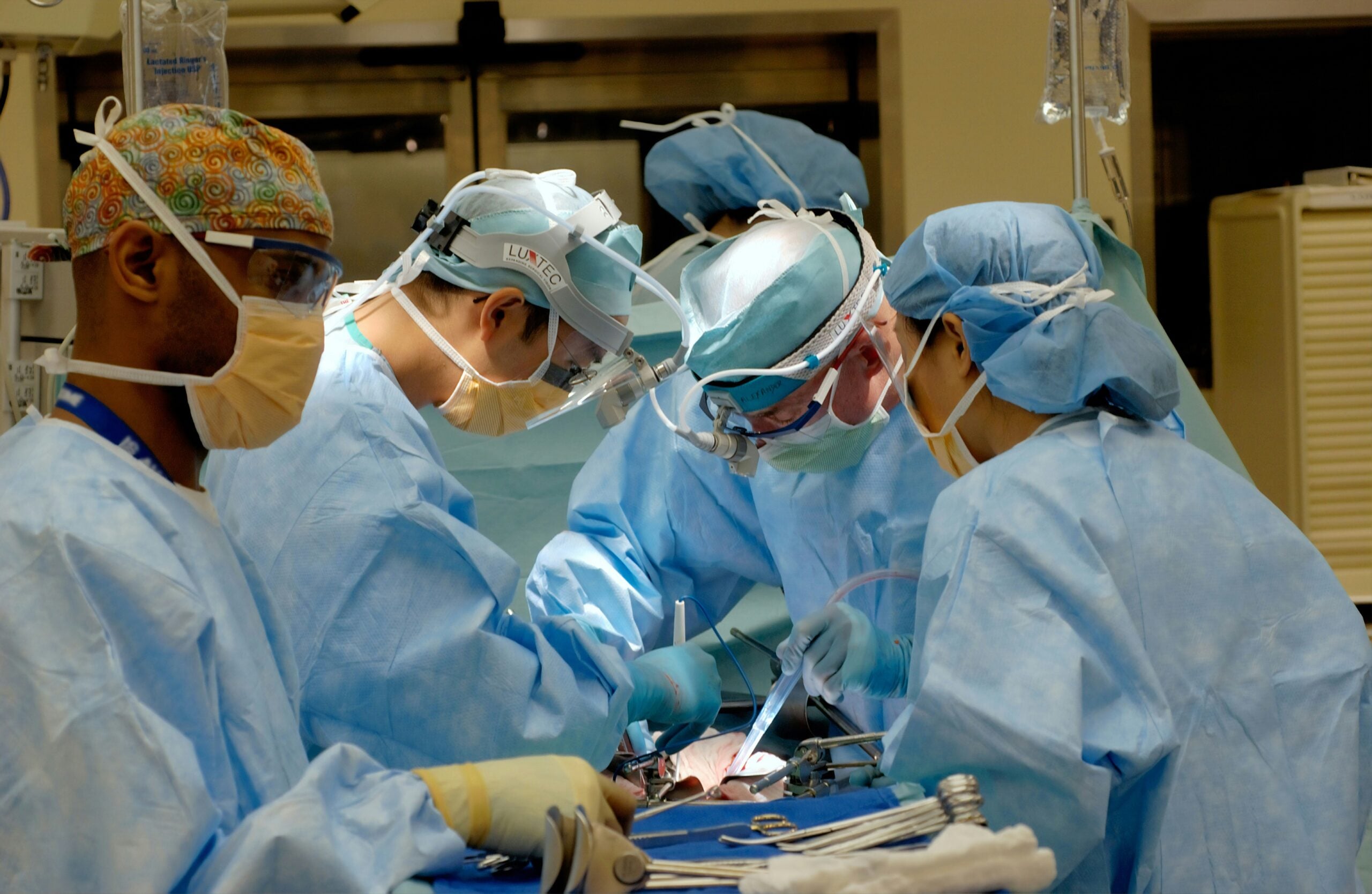
Some plans want you to start with a primary care provider (PCP) and get referrals before seeing certain specialists. Jumping straight to a specialist without that referral can mean denied claims or higher out-of-network-style costs.
Before you book a specialist on your own, glance at your plan rules:
- Do you need a PCP referral?
- Does the specialist need to be in a certain network tier?
A two-minute check can save you from a bill that only shows up months later.
*This article was developed with AI-powered tools and has been carefully reviewed by our editors.

Leave a Reply